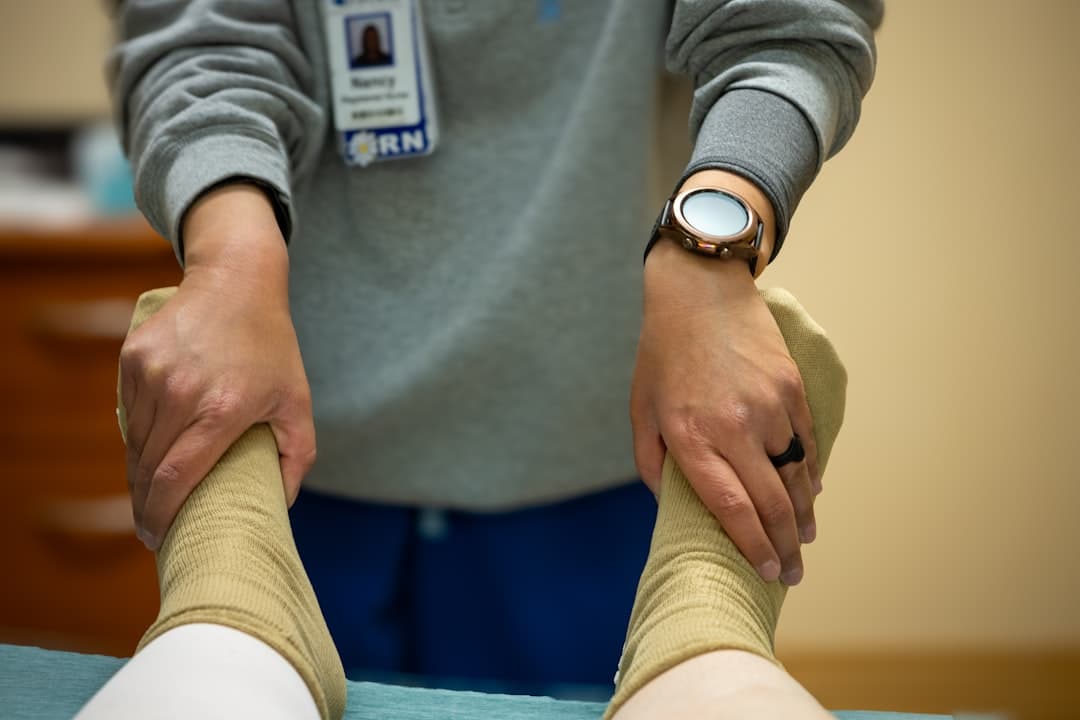
Pain After Knee Replacement: Why It Still Hurts
Summary
Persistent pain after a total knee replacement can be confusing and discouraging, especially when surgery was meant to relieve pain. This article follows the video’s practical, step-by-step approach: first rule out serious, treatable problems like infection, loosening, or fracture, then consider stiffness, referred pain from the hip or back, kneecap tracking issues, and rarely, metal allergy. It also highlights a key theme, dissatisfaction is often tied to expectations and starting pain levels. You will find action-oriented questions to ask, what tests are commonly used, and ways to reduce the odds of disappointment.
🎯 Key Takeaways
- ✓About 1 in 5 people do not fully love their knee replacement long term, even when X-rays and motion look “good.”
- ✓The first priority is ruling out treatable causes of a painful knee replacement, especially infection, loosening, and fracture.
- ✓Pain can be referred from the hip or spine, meaning the knee feels like the problem even when it is not.
- ✓Stiffness has multiple drivers, including pre-surgery range of motion and rehab barriers, and it can be painful or painless.
- ✓Unmet expectations are a major modifiable reason people feel unhappy after surgery, even when the implant is functioning.
You did the hard thing. You got a total knee replacement, you rehabbed, you waited for healing, and the knee still hurts, or it just does not feel like the outcome you hoped for.
That frustration is the starting point of the video’s message: a painful total knee replacement is real, it is common enough that you are not alone, and it deserves a careful, step-wise workup instead of a shrug.
One blunt reality anchors the whole discussion.
Research and clinical experience both suggest that a meaningful minority of people remain dissatisfied after total knee replacement, even when the implant looks fine on imaging and the knee bends reasonably well. Large reviews often cite dissatisfaction rates in the range of 10% to 20% depending on how it is measured, and the clinicians in the video summarize it as about 1 in 5 people not totally loving their knee. (For broader context, see discussion of satisfaction variability in the American Academy of Orthopaedic Surgeons patient guidanceTrusted Source.)
The hopeful part is that some causes of ongoing pain are treatable, but you have to look for them in the right order.
Pro Tip: If your knee replacement is persistently painful, bring a one-page “pain timeline” to your appointment. Include when pain started (immediately vs months later), where it is located (front, inside, outside, back), what triggers it (stairs, twisting, standing), and any fevers, wound drainage, or recent falls. That single page can speed up a thorough evaluation.
When a “successful” knee replacement still hurts
A key insight from the video is that two people can have knees that look identical on paper, similar range of motion, similar reported pain scores, and one feels thrilled while the other feels deeply disappointed.
That is not “all in your head.” Pain and satisfaction are influenced by biology, mechanics, rehab access, and expectations, plus how your brain processes pain after months or years of arthritis.
Total knee replacement is also described in the video as a salvage procedure, meaning it is used when there is not much else left to fix severe arthritis. The new joint is metal and plastic, and it can work remarkably well, but it is not the same as a natural knee.
The practical takeaway is action-oriented: if you are still hurting, treat it like a solvable puzzle until proven otherwise.
Start with the big three: infection, loosening, fracture
The video’s approach is clear: rule out the most important, correctable problems first. Even if they are less common than general dissatisfaction, they matter because missing them can delay treatment.
1) Infection
Infection is the first concern raised for any painful total knee replacement.
A prosthetic joint infection can show up early after surgery or later, and it is not always obvious. The clinicians emphasize an uncomfortable truth: even with a careful history, exam, and tests, infection can still be hard to fully rule out, and sometimes it declares itself later.
What a typical workup may include (your clinician decides what fits your case):
If an infection is found, it can be treated, but the treatment plan varies widely, from antibiotics to surgical procedures. That is exactly why it belongs at the top of the list.
Important: Seek urgent medical care if you have a knee replacement and develop fever, rapidly increasing redness or warmth, new drainage from the incision, or sudden inability to bear weight. Those symptoms can be associated with infection or other serious complications.
2) Loosening
Next on the video’s list is a loose total knee.
Loosening can happen if the implant does not bond well early on (whether cemented or uncemented), or later after trauma. A specific scenario mentioned is a fall onto a bent knee, which can stress the components.
This is a mechanical problem, and mechanical problems tend to hurt with mechanical triggers, such as weight-bearing, twisting, or repeated rising from a chair. Your clinician may look for clues on X-rays, and sometimes advanced imaging is used.
If loosening is confirmed, it is potentially correctable, but correction usually involves surgery, which is a major decision.
3) Fracture around the implant
A periprosthetic fracture is another “must not miss” cause.
The video highlights a practical issue: because the implant is metal, a fracture can be harder to see on standard X-rays if the break line hides behind the prosthesis. These fractures can occur soon after surgery or even many years later.
If you had a recent fall, a sudden new pain spike, or new deformity or instability, tell your clinician right away. Additional imaging may be needed.
Did you know? Total knee replacement is common, with hundreds of thousands performed yearly in the United States. As procedure volume rises, the absolute number of complications like infection or periprosthetic fracture also rises, even if percentages remain low. (Procedure overview: NIH MedlinePlus knee replacement informationTrusted Source.)
Stiff knees, and why range of motion matters so much
Not all painful knee replacements are infected, loose, or fractured. The video then moves into a more common, messier category: stiffness.
A stiff knee can be painful, but it can also be stiff and not very painful. That is one reason stiffness needs its own evaluation.
Why stiffness happens
The discussion offers several real-world causes, including:
This framing matters because it shifts the conversation away from blame. Stiffness is often a combination of biology, logistics, and pain control, not simply “not trying hard enough.”
What you can do with this information
If your main issue is stiffness, bring specifics:
That detail helps your care team decide whether the pattern fits swelling and deconditioning, scar tissue, mechanical limitation, or another cause.
What the research shows: Recovery after knee replacement is highly variable. Many people continue to see improvements in function and symptoms for months, and sometimes up to a year, depending on the outcome being measured. (General recovery overview: AAOS total knee replacementTrusted Source.)
When the pain is not actually from the knee (referred pain)
This is one of the video’s most distinctive points, and it is also one of the hardest for many people to accept.
Sometimes, the knee is not the true source of the pain.
The classic example given is a severely arthritic hip. A person says, “My knee hurts,” and the clinician is thinking, “It is your hip arthritis.” The patient understandably feels dismissed because the pain is felt in the knee, especially after knee surgery.
This is referred pain, meaning the brain interprets signals from one area as coming from another. The video specifically calls out two common sources:
A practical implication is huge: if the pain is referred, revising the knee may not help, because the knee is not the driver.
Action steps to discuss with your clinician if referred pain might fit:
Q: How can hip arthritis feel like knee pain?
A: Nerves that carry pain signals from the hip can overlap with areas where you feel pain around the front or inside of the knee. That means your brain may register the discomfort as “knee pain,” even when the knee implant is fine.
If your knee replacement looks stable but pain persists, it can be worth asking for a hip and spine check, especially if you also have groin pain, reduced hip motion, or back symptoms.
Talking with Docs clinicians, orthopedic perspective
Front-of-knee pain, patella tracking, and other “rare but real” causes
After the major threats and common patterns, the video moves into additional causes that can still matter a lot to the person experiencing them.
Patella (kneecap) tracking problems
The patella is highlighted as a potential source of front-of-knee pain, especially if it does not track properly, for example drifting to the outside.
Even with “perfect” tracking, some people still experience anterior knee pain that can be difficult to solve. This is an important nuance: not every pain source has a clean fix, and knowing that early can prevent a cycle of escalating interventions.
Metal allergy (uncommon, hard to diagnose)
Given your provided niche label of “Allergies,” this is the one point that overlaps most directly.
The video places metal allergy low on the list, but still on the list. It may be associated with pain and swelling, and it can be difficult to diagnose. Some people may know ahead of time due to prior reactions or allergy testing.
What is worth knowing from broader medical references is that true implant allergy is considered uncommon, testing is imperfect, and symptoms can overlap with other causes such as infection or mechanical issues. If allergy is a concern, it is typically handled in partnership with orthopedics and sometimes allergy or dermatology specialists. (Background on metal allergy concepts: American Academy of Dermatology on nickel allergyTrusted Source.)
Other rare causes mentioned
The video also lists several less common, but plausible contributors:
The unifying theme is that your surgeon or second-opinion clinician should have a step-wise process that tries to rule out as many identifiable causes as possible. Sometimes you get a clear diagnosis. Sometimes you do not.
The expectations problem: why some people are happy and others are not
The video draws a line between “painful” and “unhappy,” and it treats expectations as central.
One of the most actionable claims is this: unmet expectations may be the number one modifiable risk factor for unhappiness after knee replacement.
That is not the same as saying your pain is not real. It is saying that satisfaction depends on the gap between what you hoped for and what is realistically achievable with an artificial joint.
The “paint a house” analogy
The clinicians use a memorable analogy.
Applied to knees, someone who could barely walk 20 meters before surgery may feel a huge improvement and love their new knee. Someone who could hike 10 kilometers but had pain near the end may feel less dramatic improvement and may struggle to feel satisfied, even if the surgery technically helped.
“Wait as long as you can” as a satisfaction strategy
A distinctive viewpoint in the video is the recommendation to put off surgery as long as possible, when it is safe and reasonable to do so.
The rationale is not to make you suffer. It is to increase the chance that the improvement feels meaningful, and to reduce the number of years you might live with disappointment if you are in the unlucky group with persistent symptoms.
This is not the only philosophy in orthopedics, and the video openly acknowledges that other surgeons may recommend earlier surgery. The core message is to make the decision thoughtfully, with your personal goals in mind.
Resource Callout: »MORE: Before you decide on surgery or revision, consider writing a “Top 5 activities list.” Include what you most want to do (walk the dog, stairs, gardening, travel), what you can do now, and what you consider a good result. Bring it to your surgeon or physical therapist to align expectations and rehab priorities.
How to advocate for yourself at follow-up or a second opinion
If you are still sore months or years later, the video’s closing advice is practical: rule out correctable issues, and make sure the decision-making around surgery is thoughtful.
Here is a step-by-step way to bring that approach into your next appointment.
How to prepare (a numbered plan)
Describe the pain like a mechanic, not a judge. Share location, triggers, timing, swelling patterns, and whether the pain is getting better, worse, or stuck. This helps separate mechanical pain from inflammatory pain.
Ask what has been ruled out, and what has not. Specifically ask whether infection, loosening, and fracture have been considered and what tests support that conclusion.
Bring up referred pain directly. Ask whether your hip and back have been evaluated as possible sources. If you have groin pain, buttock pain, numbness, or shooting pain, mention it.
Clarify the goal of any next step. If a test is ordered, ask, “What are we looking for?” If a procedure is proposed, ask, “What problem is this meant to solve?”
Revisit expectations in concrete terms. Ask what activities are realistic, what level of discomfort is common, and what timeline is expected for improvement.
A practical question list to bring with you
Q: If my X-ray looks fine, does that mean nothing is wrong?
A: Not necessarily. Some problems are not obvious on standard X-rays, and pain can also come from outside the knee, such as the hip or spine. A “normal” X-ray is reassuring, but it is only one piece of the puzzle.
A step-wise evaluation that considers infection, loosening, fracture, stiffness, referred pain, and kneecap mechanics can help narrow down what is most likely.
Talking with Docs clinicians, orthopedic perspective
Key Takeaways
Frequently Asked Questions
- How common is it to be unhappy after a total knee replacement?
- The video’s clinicians summarize it as about 1 in 5 people not totally loving their knee replacement. Broader research also suggests a minority of patients report dissatisfaction, even when the implant appears to function well.
- What is the first thing doctors try to rule out with a painful knee replacement?
- Infection is typically the top concern because it can be serious and may be treatable if identified. Evaluation often includes a history and exam, blood tests for inflammation, and sometimes aspiration of joint fluid.
- Can hip arthritis really cause knee pain after knee replacement?
- Yes. Referred pain can make hip arthritis feel like knee pain, which is why a hip exam and sometimes imaging may be appropriate when the knee implant looks stable but symptoms persist.
- Is metal allergy a likely cause of pain after knee replacement?
- The video describes metal allergy as real but uncommon and difficult to diagnose. If it is a concern, it is usually considered after more common causes like infection, loosening, fracture, stiffness, and referred pain have been evaluated.
- If my knee is stiff after surgery, does that mean something went wrong?
- Not always. Stiffness can relate to pre-surgery range of motion, swelling, pain control, and rehab access, among other factors. A clinician can help determine whether the stiffness pattern suggests scar tissue, mechanics, or another cause.
Get Evidence-Based Health Tips
Join readers getting weekly insights on health, nutrition, and wellness. No spam, ever.
No spam. Unsubscribe anytime.