Hyperbaric Oxygen Therapy for Longevity: A Reality Check
Summary
Hyperbaric oxygen therapy (HBOT) is often framed as a niche treatment for athletes or stroke recovery, but this video puts it in a longevity spotlight. After 5,400 minutes in a pressurized oxygen chamber (60 sessions in 90 days), the speaker reports surprisingly broad changes, including no detectable inflammation on bloodwork, a 28.6% drop in a cognitive decline marker tied to Alzheimer’s risk, improved microbiome results, better skin health, and longer telomeres. This article investigates those claims, highlights common misconceptions, and explains what research and medical guidance actually support, plus practical questions to ask your clinician.
Hyperbaric oxygen therapy, or HBOT, sits at an unusual intersection of respiratory physiology and modern longevity culture.
It matters because oxygen is not just “fuel” for breathing. Oxygen delivery influences how tissues respond to injury, infection, and inflammation, and those same processes are often linked to broader outcomes like cardiovascular risk and cognitive health.
Why HBOT suddenly matters beyond the lungs
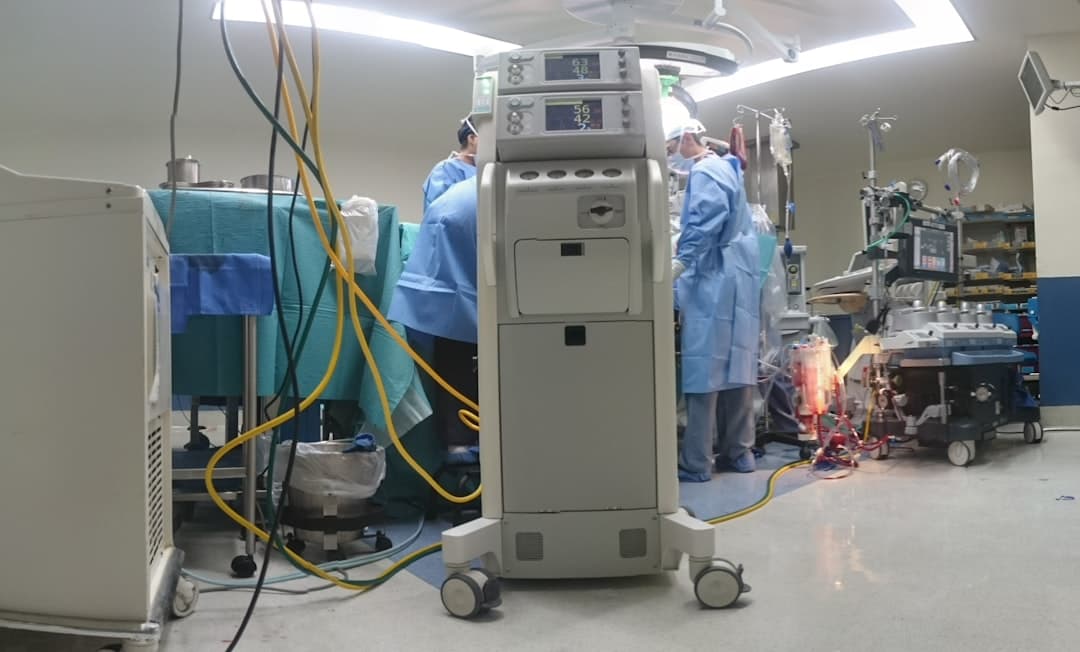
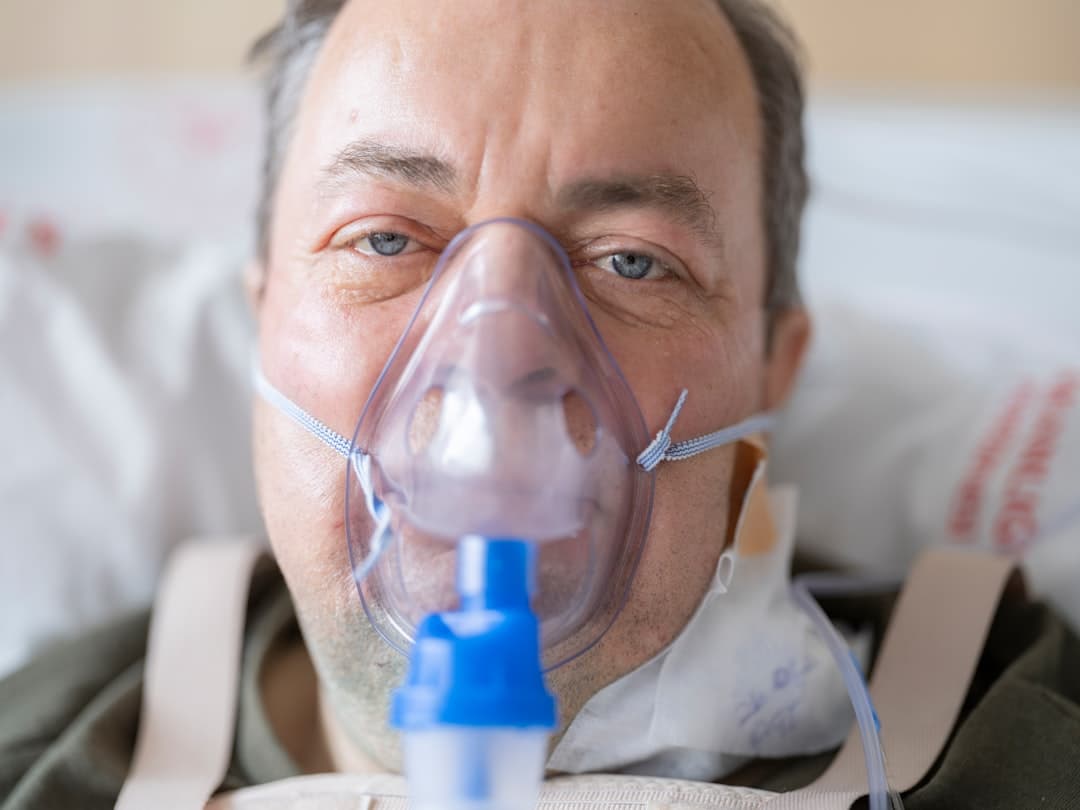
HBOT is simple to describe and easy to misunderstand. You sit in a pressurized chamber and breathe near-100% oxygen. The pressure helps dissolve more oxygen into your blood plasma, not just onto hemoglobin, which can increase oxygen availability to tissues.
That respiratory twist is why HBOT is used in mainstream medicine for specific indications. The FDA lists several accepted uses, such as decompression sickness and certain hard-to-heal wounds, among others (FDA overview of hyperbaric oxygen therapyTrusted Source).
Did you know? Some “oxygen” services marketed for wellness are not medical HBOT. The FDA warns that unproven claims are common, and the device and setting matter for both safety and results (FDATrusted Source).
Inside the video’s self-experiment: 5,400 minutes of oxygen
The video’s unique perspective is investigative and personal: the speaker logs 5,400 minutes in a pressurized tank to spare viewers the guesswork. The protocol is also unusually concrete for a social media claim, 60 sessions in 90 days.
The reported outcomes are broad. Bloodwork allegedly showed no detectable inflammation, and a marker associated with cognitive decline and Alzheimer’s risk dropped by 28.6%. The speaker also reports that their microbiome improved dramatically, skin health improved, and even telomeres lengthened.
Those are attention-grabbing endpoints because they span multiple systems, immune signaling, brain health proxies, gut ecology, dermatology, and cellular aging.
What the research shows: HBOT is being studied for a range of conditions beyond its established uses, but evidence quality varies by condition, and “longevity” outcomes are not yet settled. For example, clinical guidance and summaries note clear roles in selected medical problems while broader wellness claims remain less certain (Mayo ClinicTrusted Source).
Misconceptions vs what HBOT can realistically do
Misconception 1: More oxygen always equals better health. Oxygen can be therapeutic, but it is also biologically active. Too much oxygen exposure under pressure can raise the risk of side effects in some people, which is why medical screening and supervision are emphasized in clinical settings (Mayo ClinicTrusted Source).
Misconception 2: Biomarker changes automatically mean longer life. This is the key investigative tension in the video. Inflammation markers, cognition-linked biomarkers, microbiome readouts, and telomere length can change for many reasons, including sleep, training load, infections, weight changes, medications, and lab variability. A single-person experiment can be inspiring, but it cannot separate HBOT from everything else happening over 90 days.
Misconception 3: HBOT is the same everywhere. There are different chamber types and pressure protocols. Clinical HBOT is not identical to every “mild hyperbaric” or spa offering, and the difference can matter.
Important: If you have lung disease, a history of collapsed lung, frequent ear or sinus problems, or you are pregnant, do not assume HBOT is automatically safe. Ask a clinician who can review your personal risks and medications.
If you are considering HBOT, ask these questions first
A practical way to use the video is as a checklist for better decision-making, not as a promise.
What is the goal, and how will we measure it? Define what “working” means, such as wound healing progress, symptom tracking, or specific labs, and decide timing for repeat measurements.
What exact protocol is being offered? Ask about chamber type, pressure, session length, number of sessions, and who supervises.
What are the most relevant risks for me? Ear barotrauma, sinus pressure, and oxygen-related side effects may be more likely in certain people, and your clinician can help weigh benefit vs risk.
Pro Tip: If a clinic promises “guaranteed anti-aging” or “reverses Alzheimer’s,” treat that as a red flag. Ask for condition-specific evidence and realistic outcomes instead.
Key Takeaways
Frequently Asked Questions
- Is hyperbaric oxygen therapy proven for longevity?
- HBOT is proven for certain medical indications, but using it primarily for longevity is still an emerging area with mixed evidence. If you are considering it for wellness goals, discuss realistic outcomes, costs, and safety screening with a qualified clinician.
- What does a “pressurized oxygen chamber” actually do?
- In HBOT, you breathe near-100% oxygen while the chamber pressure is increased, which can raise the amount of oxygen dissolved in your blood plasma. That higher oxygen availability may support specific healing processes in select conditions, typically under medical supervision.
Get Evidence-Based Health Tips
Join readers getting weekly insights on health, nutrition, and wellness. No spam, ever.
No spam. Unsubscribe anytime.