5 Things to Do Before Your Next Blood Test
Summary
Blood work can feel routine, but small choices before the draw can change both your experience and what your results mean. This article follows a clinician’s practical, slightly unconventional approach: make the draw physically easier (better veins, less needle discomfort) and make the data more useful (consider both fasted and post-meal labs). You will learn why arm training can improve venipuncture success, how a butterfly needle may reduce discomfort, and how a “metabolic stress test” style, non-fasted lab can reveal how your body handles the foods you actually eat.
Blood work is one of those health rituals that can feel both ordinary and oddly emotional.
One minute you are “just getting labs,” the next you are watching vials fill, hoping the needle goes in cleanly, and wondering whether that number on the report actually reflects your day-to-day health.
This video’s unique perspective is practical in a way many lab guides are not. It focuses on two things people rarely connect: making the blood draw easier on your body, and making the results more informative about your real life.
And yes, it includes a refreshingly specific request you can make at the chair.
Why “how you test” can matter as much as “what you test”
A common misconception is that lab results are purely about your biology, as if the test happens in a vacuum.
In reality, lab values can shift based on timing, meals, recent exercise, stress, and even how difficult the draw is.
The discussion highlights a simple goal: use blood work to track health trends over time, not just to collect one-off numbers. That is why the speaker talks about building a baseline, then later adding a more “real-world” challenge test using your normal meal.
There is also a second goal that deserves attention: reduce the friction that makes people avoid labs. If you have ever felt faint, nauseated, or embarrassed during a draw, you are not alone. Needle fear and vasovagal reactions are common, and they can be triggered by pain, anxiety, or even just the sight of blood.
Did you know? Feeling lightheaded or faint during a blood draw is often related to a vasovagal response, a reflex that can lower heart rate and blood pressure. The Cleveland ClinicTrusted Source explains common triggers and what it can feel like.
This framing is not about “toughing it out.” It is about making the process more predictable and more useful.
Tip 1: Build better veins before the appointment
The first tip is almost sneaky: exercise can make venipuncture easier.
The idea is straightforward. When you are physically fit, especially if you train your arms, veins may be more visible and easier to access. That can mean fewer pokes, less digging, and a faster draw.
What is interesting about this approach is that it treats “good veins” as something you can train for, not something you either have or do not have.
What “work out your arms” can look like
The speaker mentions pumping the wrists and fingers and, more broadly, building arm fitness over time.
They also call out blood flow restriction training as a way some people may bring more vascularity closer to the surface after training for a couple of months.
If you are considering blood flow restriction training, it is worth being cautious. It can be safe for some people when done correctly, but it is not for everyone, especially those with certain cardiovascular or clotting risks. If you have medical conditions or take blood thinners, it is smart to check with a clinician first.
Here are practical, low-drama ways to support easier draws without trying to “hack” your body overnight:
Pro Tip: If you tend to have “hard sticks,” ask the lab if you can sit for a few minutes with a warm pack on your inner elbow before the draw.
Tip 2: Ask for a butterfly needle (and know what that means)
This is the tip many people have never heard, even if they have had dozens of blood tests.
The recommendation is to request a butterfly needle.
A butterfly needle setup often uses a smaller gauge needle and flexible tubing, which can make the experience feel less intense for some people. In the video, the speaker contrasts a typical larger needle with a butterfly that is “two to three gauges smaller.” They describe feeling nauseated when a larger needle shifts in the vein while multiple tubes are being swapped.
One detail the speaker emphasizes is a common point of confusion: in needle sizing, smaller gauge numbers mean larger needles.
The video gives concrete examples:
This is not about being “dramatic.” The speaker even shares a personal story of fainting during blood donation and how embarrassing it felt. That matters because it normalizes the experience and offers a practical solution you can ask for.
Important: Not every lab can use a butterfly needle for every test, and not every vein is appropriate for it. If a phlebotomist recommends a different setup for safety or sample quality, ask them to explain their reasoning and follow their guidance.
What to say at the chair
You do not need a speech.
Try a simple request: “I tend to get lightheaded with blood draws. Could we use a butterfly needle if possible?”
If you have fainted before, mention it early so they can position you safely, for example lying down.
Expert Q&A
Q: I have fainted during blood draws. What can I do besides ‘being brave’?
A: Tell the staff before the needle comes out, and ask if you can lie down for the draw. Many people do better with a butterfly needle, slow breathing, and staying hydrated (if allowed for your test). If fainting is frequent or severe, discuss it with your clinician so other causes can be considered.
Video clinician, health educator
Tip 3: Start with fasted labs to set a baseline
The fasted versus fed question is where this video becomes more than “how to survive a needle.”
The recommendation is nuanced: if you have never had labs, or it has been years, do your first draw fasted.
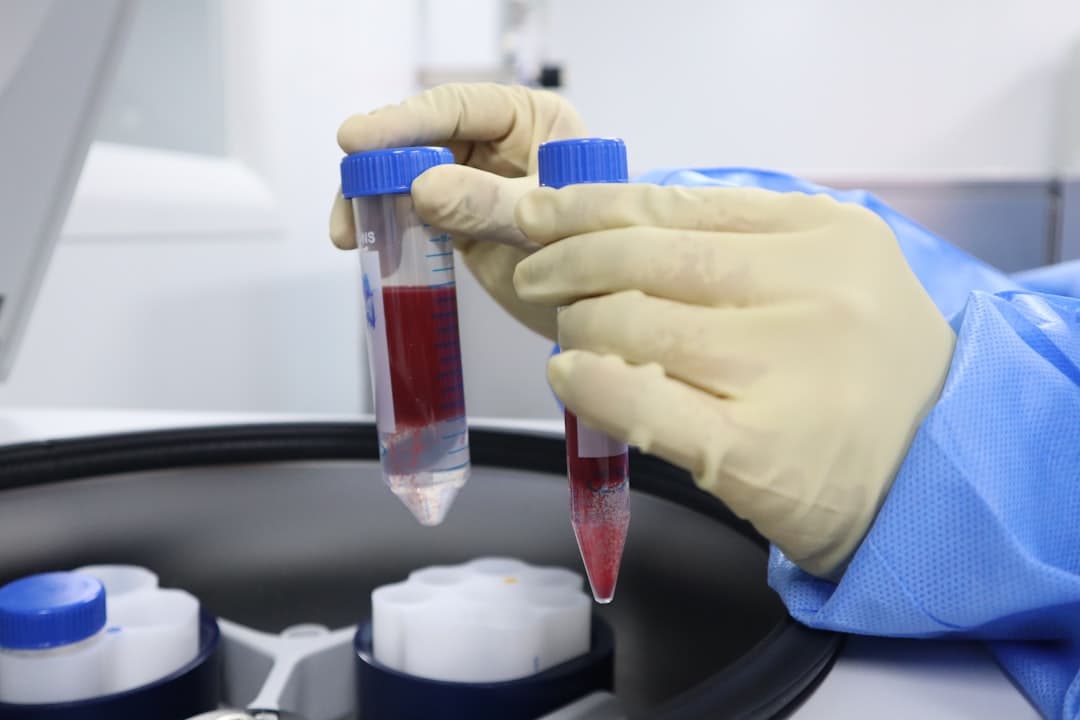
A fasting baseline can help interpret markers like fasting glucose, fasting insulin, and fasting triglycerides. It also gives you a stable reference point for comparing future tests.
This perspective aligns with how many clinicians use fasting labs in metabolic health assessments. For example, lipid testing has historically been done fasting, although many guidelines now allow non-fasting lipids in certain situations. The American Heart AssociationTrusted Source explains why fasting may still be recommended in some cases, such as when triglycerides are high or when specific follow-up testing is needed.
The speaker also lists a broader set of biomarkers they like to track over time, including:
Not everyone needs every marker. The key insight is the intent: pick a reasonable set, then repeat it consistently enough to see direction over time.
Tip 4: Then consider a non-fasted “metabolic stress test” draw
Here is the video’s most distinctive idea: once you have a baseline, consider doing non-fasted labs on purpose.
This view holds that fasting labs can miss how your body handles the meals you actually eat.
Instead of treating food as “noise” that ruins the test, the speaker treats food as the stimulus that reveals metabolic flexibility.
The timing and the meal are specific
The suggested protocol is simple and realistic:
This is essentially a DIY mixed-meal challenge, not a formal oral glucose tolerance test.
The speaker’s reasoning is memorable: atherosclerosis does not develop only in the fasted state. Many metabolic stressors happen after meals, when triglyceride-rich lipoproteins rise and insulin has to manage incoming nutrients.
What the research shows: Post-meal triglycerides, sometimes called non-fasting triglycerides, are increasingly recognized as meaningful for cardiovascular risk assessment. A scientific statement from the American Heart AssociationTrusted Source discusses triglycerides and their role in atherosclerotic cardiovascular disease.
This does not mean you should change your clinician’s instructions. Some tests require fasting, and some medications should not be paused. It means there may be value in planning certain follow-up labs in a fed state, if your healthcare professional agrees.
Why this can uncover misconceptions
A common misconception is, “My fasting labs are fine, so my metabolism is fine.”
Sometimes that is true.
But some people can maintain normal fasting glucose while still having exaggerated post-meal spikes in glucose or insulin, especially early in insulin resistance. The National Institute of Diabetes and Digestive and Kidney DiseasesTrusted Source explains different tests used to evaluate diabetes and prediabetes, and why multiple measures can matter.
Another misconception is that a single “healthy” meal works the same in every body.
This approach invites curiosity: how does your body handle the nutrients you habitually eat when you are not in a fasting bubble?
Resource callout
»MORE: Bring a one-page “lab day plan” to your appointment, including whether you are fasting, your usual meal choice if doing a fed draw, your timing (90 to 120 minutes), and any history of fainting.
A quick reality check before you try it
Non-fasted testing is not a free-for-all.
If your clinician ordered fasting labs, follow those instructions, then ask whether a separate, planned non-fasted panel could be useful later. Also consider consistency. If you are going to compare fed labs over time, try to keep the meal and timing similar each time.
Expert Q&A
Q: What should I eat for a non-fasted lab, a special test meal?
A: The video’s suggestion is to eat the meal you normally choose and consider “healthy for you,” then test 90 to 120 minutes after finishing. That way, the results reflect your real dietary pattern rather than a one-time experiment. If you have specific conditions like diabetes, ask your clinician what is safe and appropriate.
Video clinician, health educator
Key Takeaways
Frequently Asked Questions
- Can I request a butterfly needle for any blood test?
- You can ask, and many labs can accommodate it, especially if you have small veins or a history of fainting. However, the phlebotomist may recommend a different needle based on vein size, required sample volume, or test requirements.
- Should I always do my blood work fasting?
- Not always. Fasting can be helpful for establishing a baseline, but some non-fasted values can also be clinically useful. Follow your clinician’s instructions, and ask whether a planned fed draw could add information later.
- How long after eating should I do a non-fasted lab draw?
- The video suggests aiming for a blood draw 90 to 120 minutes after finishing your usual meal. Timing matters, so try to be consistent if you repeat this approach.
- What if I get dizzy or faint during blood draws?
- Tell the staff before the draw, and ask to lie down if possible. Many people find that hydration (if allowed), slow breathing, and using a smaller needle setup can help, but frequent fainting should be discussed with a clinician.
Get Evidence-Based Health Tips
Join readers getting weekly insights on health, nutrition, and wellness. No spam, ever.
No spam. Unsubscribe anytime.