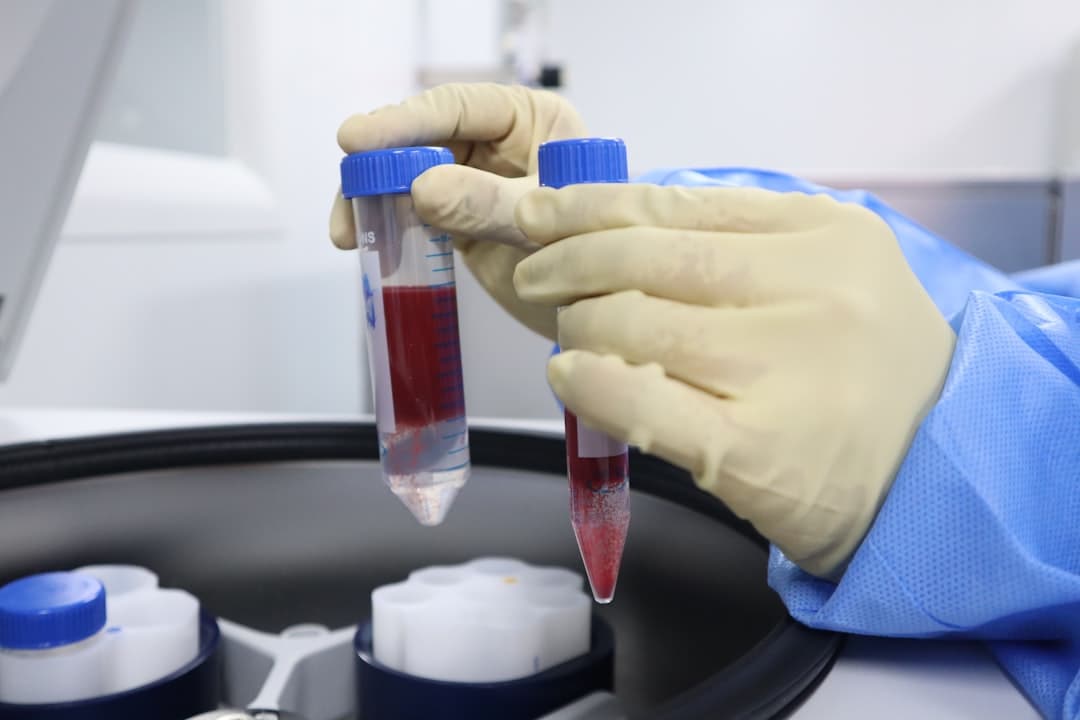
Bloodwork Red Flags That Hide in Plain Sight
Summary
Some of the most important bloodwork clues are not “abnormal” in isolation, they become meaningful when you connect them. In this lab review, the key pattern is a mix of higher ferritin, thicker-blood signals (hemoglobin, hematocrit, fibrinogen), elevated Lp(a), and metabolic markers (triglycerides, ApoB:A1 ratio) that may amplify cardiovascular risk. The approach emphasizes practical levers: repeat testing before panicking, consider hydration and blood donation with clinician guidance, improve metabolic flexibility with walking and resistance training, reduce processed carbs, and take sleep and possible sleep apnea seriously. Low DHEA is discussed as a potential sleep and stress axis clue.
🎯 Key Takeaways
- ✓Ferritin around 463 ng/mL is framed as a “pause and recheck” finding because it can rise with inflammation or illness, but persistently high levels deserve follow-up.
- ✓Blood thickness signals (hemoglobin 16 g/dL, hematocrit 47.2%, fibrinogen 309 mg/dL) are treated as more concerning when combined with elevated Lp(a).
- ✓Lp(a) 83 nmol/L is discussed as a risk amplifier, with a notable link to sleep-disordered breathing as a possible contributor to investigate.
- ✓Triglycerides (110 mg/dL) and an ApoB:A1 ratio closer to 1 (about 0.8) are used as a “metabolic health” lens, even with a good A1C (5.1%).
- ✓The practical “three knobs” model is exercise, intermittent fasting, and carbohydrate quality and quantity, with walking after higher-carb meals to blunt post-meal glucose spikes.
- ✓Low DHEA is positioned as a stress and sleep-adjacent marker, with an example dosing heuristic (10 mg per decade of life) to discuss with a clinician.
The most useful bloodwork insight in this lab review is simple: risk often hides in combinations, not in a single lab value.
This is framed through one person’s labs, a dad with two kids and another on the way, and the goal is accountability rather than alarm. The interesting part is how several “borderline” markers can stack together into a clearer signal about inflammation, blood viscosity, metabolic flexibility, and sleep.
Important: If you try to interpret labs on your own, you can miss context like altitude, recent illness, medications (including testosterone therapy), hydration status, and family history. Use this as a discussion guide for your next clinician visit, not as a diagnosis.
The big takeaway: patterns matter more than one “bad” number
A single lab can be noisy. A pattern is harder to ignore.
The discussion highlights a common health puzzle: someone can look “pretty healthy” on the surface, even have a strong A1C, and still show a cluster of markers that suggest higher cardiovascular strain when viewed together.
In this case, the cluster includes:
What’s nuanced about this approach is the refusal to obsess over any single marker. The suggestion is to ask, “What is the body doing overall, and what are the easiest levers to pull first?”
»MORE: If you keep copies of your labs, consider building a one-page “trend sheet” with dates and the same markers each time (ferritin, CBC, lipids including triglycerides, ApoB, Lp(a), A1C). Trends often tell a clearer story than one snapshot.
Ferritin 463: stored iron, inflammation, and the “rerun first” mindset
Ferritin is the stored form of iron, but it is also an acute phase reactant (a marker that can rise during inflammation). That matters because ferritin can jump after infections, intense training blocks, heavy alcohol intake, and other inflammatory hits.
So the first move here is not panic, it is confirmation.
Why “rerun labs” can be the smartest first step
The recommendation is to rerun the labs to save money and reduce unnecessary workups, unless there is a known history of ferritin living in the 400s. This is a practical point many people skip. If you had COVID, the flu, or another inflammatory event near the blood draw, ferritin can be misleading.
At the same time, the concern is not theoretical. Persistently high iron stores can matter, and the speaker flags a link between high ferritin or iron and neurodegenerative outcomes like dementia and Alzheimer’s disease (as a risk association, not a guarantee).
If ferritin remains elevated, one condition clinicians often consider is hereditary hemochromatosis, an iron overload disorder. A typical medical workup may include repeat ferritin, transferrin saturation, and sometimes genetic testing, depending on context. You can read an overview of hemochromatosis evaluation from the U.S. National Library of MedicineTrusted Source.
Did you know? Ferritin can rise even when iron overload is not the problem, because ferritin is also part of the body’s inflammatory response. That is one reason clinicians often interpret ferritin alongside other iron studies, liver enzymes, and clinical history.
Blood viscosity clues: hemoglobin, hematocrit, and fibrinogen together
Thickness is not a diagnosis, it is a risk context.
The discussion points to hemoglobin of 16 g/dL and hematocrit of 47.2% in someone living at sea level, plus testosterone on the higher side (with uncertainty about whether hormone therapy is involved). On their own, these numbers may fall within many lab reference ranges. The key idea is that they might still matter if they contribute to higher blood viscosity in a person who already has other cardiovascular risk amplifiers.
Then there is fibrinogen at 309 mg/dL, framed as another “blood stickiness” or clotting-adjacent marker. Fibrinogen is involved in clot formation and is also an inflammatory marker. Higher fibrinogen levels have been associated with cardiovascular risk in population studies, although it is not used alone to diagnose disease. For background, the American Heart Association describes fibrinogen as one of several factors that can influence clotting and cardiovascular risk in broader discussions of thrombosis and atherosclerosis, see AHA resourcesTrusted Source.
The practical suggestions raised in the video
This is where the recommendations get very concrete, and also where you should loop in a clinician.
Pro Tip: If you are repeating labs because of high hemoglobin, hematocrit, or ferritin, try to standardize the week before the test. Similar hydration, similar training intensity, similar alcohol intake, and no testing during an acute illness if you can avoid it.
Lp(a) 83 nmol/L: why sleep may be part of the cardiovascular puzzle
Lp(a) is treated here as a risk amplifier, especially when other metabolic markers are not ideal.
Lp(a), or lipoprotein(a), is largely genetically determined, and many people will not change it dramatically with lifestyle alone. Major cardiology organizations recognize Lp(a) as an independent cardiovascular risk factor, see the American Heart Association overviewTrusted Source.
What makes this video’s perspective stand out is the sleep connection. There is an association raised between sleep-disordered breathing, including sleep apnea, and higher Lp(a). The implication is not that sleep apnea “causes” Lp(a), but that sleep may be part of the broader cardiometabolic stress picture.
Sleep-disordered breathing as a “hidden lever”
Sleep apnea can fragment sleep, raise sympathetic stress signaling, and worsen insulin resistance in some people. Over time, that may push lipids and inflammation in the wrong direction.
The speaker mentions mouth taping as something that “can be great,” but also emphasizes that other factors could be at play. The practical takeaway is to avoid assuming one hack solves a physiology-level issue.
If you suspect sleep apnea (snoring, witnessed pauses in breathing, waking up unrefreshed, morning headaches, daytime sleepiness), it is reasonable to ask a clinician about screening. The gold standard diagnostic pathway often involves home sleep apnea testing or an in-lab sleep study. For a plain-language overview, see NHLBI’s sleep apnea pageTrusted Source.
What the research shows: Treating obstructive sleep apnea can improve blood pressure and daytime sleepiness in many people, and may improve some cardiometabolic markers depending on adherence and baseline risk, according to summaries from the American Academy of Sleep MedicineTrusted Source.
Metabolic health lens: triglycerides, ApoB:A1 ratio, and the “three knobs”
Metabolic flexibility is the engine in this model.
Even with an A1C of 5.1%, which is excellent, the discussion leans heavily on fasting triglycerides and lipoprotein ratios as early warning signals. Triglycerides are described as a favorite marker by multiple lipid-focused clinicians, and the “ideal world” target offered is straightforward: HDL higher than triglycerides.
That is not a universal rule, and it is not always achievable, but it is a useful directional goal.
Why triglycerides of 110 mg/dL got attention
Triglycerides at 110 mg/dL are not extremely high, but they are not “metabolically pristine” in the framing used here. Total cholesterol is 229, VLDL is 20 mg/dL, and the overall pattern is interpreted as room for improvement.
A key mechanism is highlighted: high-glycemic, processed carbohydrates can be converted into lipids through de novo lipogenesis (the body turning excess carbohydrate energy into fat). This is one reason the argument here is that “the easiest way to lower lipid levels is to cut out carbs,” specifically processed carbs and sugars, while also exercising.
For broader context on triglycerides and cardiometabolic risk, see the CDC overview of triglyceridesTrusted Source.
The “three knobs” model (practical, not perfect)
This approach frames lifestyle change as adjusting three main levers:
A small but actionable tactic is also emphasized: walking after a higher-carb meal. Even a brisk walk can help blunt post-meal glucose spikes for many people. For background on how physical activity helps improve insulin sensitivity and cardiometabolic health, see guidance from the American Diabetes AssociationTrusted Source.
A simple “weekend donut” strategy
The framing is realistic: if you choose to have a donut with your partner or kid, consider a hike before or after, or even a walk.
That is not a free pass, but it is a way of thinking in systems. Food choices, movement, and timing interact.
Q: If my A1C is normal, do I still need to care about triglycerides and ApoB?
A: A1C is a valuable long-term glucose marker, but it does not capture everything about metabolic health. Triglycerides and ApoB-related markers can reflect how your body is handling energy and lipoprotein traffic, sometimes shifting before A1C changes.
If you see triglycerides creeping up, it can be a useful prompt to review processed carb intake, alcohol, sleep, and activity patterns with your clinician.
Health educator perspective, based on the video’s metabolic framing
DHEA, cortisol, and sleep: a hormone angle that often gets ignored
Low DHEA is treated as a sleep and stress-axis clue, not a standalone problem.
DHEA is discussed as being on the low side, and the speaker recommends DHEA supplementation. The specific heuristic given is 10 mg per decade of life, for example 40 mg at night for a 40-year-old male.
This is a strong, specific suggestion, so it deserves extra caution. DHEA can affect hormone-sensitive conditions, interact with medications, and alter lab values. If you are considering DHEA, it is worth discussing with a clinician and rechecking levels after any change.
Why take it at night in this model?
The key rationale offered is that DHEA may antagonize cortisol, particularly at night. Cortisol is framed as the one hormone that does not decline with age, instead it can trend higher, which may contribute to worse sleep quality over time.
This is a simplified model, but it points to a real issue: sleep often becomes lighter and more fragmented with age, and stress physiology can play a role.
For a general overview of DHEA, including potential benefits, risks, and side effects, see MedlinePlus on DHEATrusted Source.
Pulling the whole plan together
The recommendations for this individual are bundled, not isolated:
The overall wellbeing link is the point: sleep, metabolism, inflammation, and cardiovascular risk often move together.
Key Takeaways
Frequently Asked Questions
- Is high ferritin always iron overload?
- No. Ferritin is a stored-iron marker, but it also rises with inflammation or recent illness. If it stays high on repeat testing, a clinician may consider additional iron studies (like transferrin saturation) to clarify the cause.
- Why would someone care about Lp(a) if LDL is the main cholesterol number?
- Lp(a) is a genetically influenced lipoprotein that can increase cardiovascular risk independently of LDL. Knowing it is elevated can change how closely you and your clinician monitor overall risk and other modifiable factors.
- Can walking after meals really affect triglycerides?
- Post-meal activity can help reduce postprandial glucose spikes and improve insulin sensitivity over time. That metabolic shift may support healthier triglyceride levels, especially when paired with fewer processed carbs and consistent exercise.
- Is DHEA safe to take at night?
- DHEA can affect hormones and is not right for everyone, especially people with hormone-sensitive conditions or certain medications. If you are considering it, it is best to discuss dosing and monitoring with a clinician and recheck labs after changes.
Get Evidence-Based Health Tips
Join readers getting weekly insights on health, nutrition, and wellness. No spam, ever.
No spam. Unsubscribe anytime.